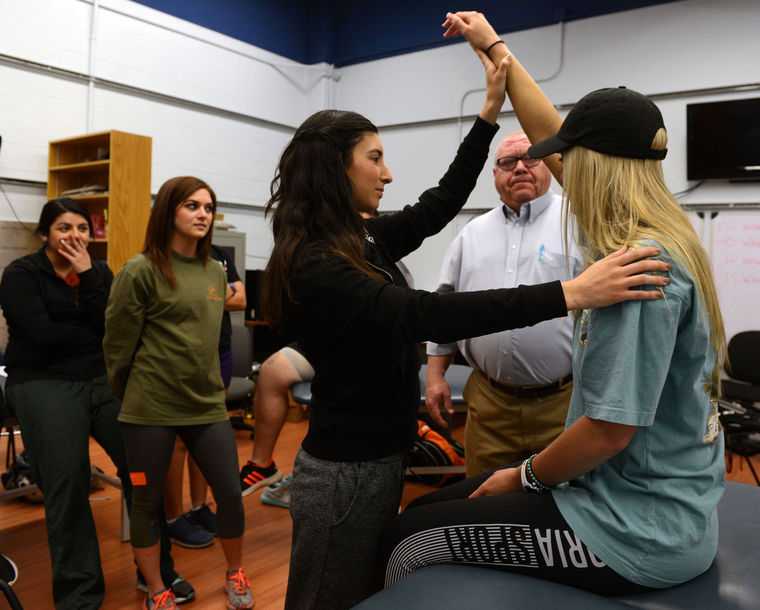Article reposted from Algor1thms for Innovation
Author: Kirstin Roundy
Scanning this glossy photo, it doesn’t look like we have a gender problem: A dozen young female scientists are striving and thriving, tackling medical problems from how burns transform fat to the relationship between the microbiota and immunity.
But when you consider the odds they faced just to get here, their accomplishments seem even more remarkable.
Women comprise half of medical school graduates and the same share of residents. Those numbers start to drop once training ends, however. Approximately 38 percent of full-time faculty members are women (40 percent at the University of Utah), but just one in five are full professors. And even fewer—16 percent—are deans.
And when it comes to clinical care, the disparity is even more acute: Women comprise 78 percent of the overall health care work force, make 80 percent of the health care decisions for their families, and represent three-fourths of family and informal caregivers. Still, just 18 percent of hospital CEOs are women (one in 10 in Utah).
Medicine isn’t alone; gender diversity lags in the “hard” sciences generally. In 2014, women earned 39 percent of the bachelor’s degrees awarded in the physical sciences (down three points from 10 years earlier). These basic scientists—chemists, biologists, molecular physicists—form the foundation of medical research. Making these cohorts more representative of the population at large is critical.
“We need a diverse biomedical workforce, because different people will bring different questions and different solutions,” says University of Utah Health Sciences Associate Vice President for Health Equity and Inclusion Ana Maria Lopez, M.D., MPH. “Greater diversity allows for better answers to the complex problems that we are facing and, ultimately, better care for our patients.”
The reasons women are not better represented in the ranks of professional mathematicians, engineers and physicians are complex and thorny. Besides decades of overt and unconscious bias, “soft” barriers also have thwarted efforts to achieve gender parity: a lack of role models and mentors, inflexible schedules, lower salaries, non-collaborative environments, and perceived bias toward male faculty (women physicians are paid 45 percent less than their male colleagues and receive half the research funding).
But while pinpointing the causes of the imbalance can be problematic, the results are undeniable: lost perspectives, unexplored research topics and missed opportunities. Those values can’t be allowed to slip away, says University of Utah Health Sciences Senior Vice President Vivian S. Lee, M.D., Ph.D., M.B.A.
“We have a responsibility to make sure the path is open for talented scientists—who also happen to be women—to succeed in our system,” says Lee. “Broad perspectives and diverse opinions lead to better thinking and nimbler problem-solving.”
Of course, combatting long-standing social and structural imbalances takes time. At University of Utah Health, shifting to gender equity is a core value. Last year, the Journal of the American Medical Association (JAMA) highlighted our efforts: We are training hiring committees to consider their own unconscious bias. We standardize interview questions and job offer letters. Every year, we analyze salaries. And we’re adjusting tenure and promotion policies to make it possible for women, and men, to take paid parental leave without being penalized.
Meanwhile, our junior faculty mentoring program has resulted in extramural funding rates of more than 90 percent for all participants. What will this mean for health care? In the end, Lee says, a diverse cohort of research scientists on the leading edge of medical innovation will result in better care. “This is about anticipating the needs of our patients, taking better care of them and improving their health along the way.”
That’s why this year’s Algorithms for Innovation features these 12 junior faculty members. From across the health sciences—the College of Nursing to Huntsman Cancer Institute—these women researchers are exploring questions ranging from placenta development to immunization rates for human papillomavirus in minority populations.
To be successful, they’ve connected with highly engaged mentors, maximized their research dollars and lifelong learning opportunities, and found or changed professional environments that match their need to balance the demands of work and life.
And we’re all better for it.

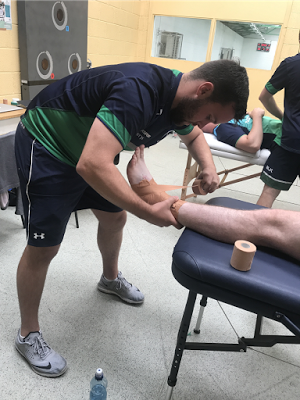
CHARLIE HICKS-LITTLE, PH.D.
ASSOCIATE PROFESSOR OF PHYSICAL THERAPY AND ATHLETIC TRAINING
DIRECTOR OF THE SPORTS MEDICINE RESEARCH LABORATORY
For Charlie Hicks-Little, her interest in research began with lacrosse. She was curious as to why several of her collegiate lacrosse teammates had torn their anterior cruciate ligament (ACL) in situations where there was no outside force contacting the knee. So, while pursuing a master’s degree in sports medicine, she investigated the looseness of the knee joint ligaments in female athletes during the menstrual cycle to determine whether there was a hormone effect related to the occurrence of ACL injury. This research experience spurred her interest in the knee joint further. During her PhD training in biomedical science, Hicks-Little examined the functional effects of knee osteoarthritis in patients with a history of knee injury. “Once you have injured your knee or have torn your ACL, your joint changes. The joint surfaces of the knee alter and your joint movement never really returns to normal. Consequently, there is an early onset of osteoarthritis in the knee joint.”
As an associate professor in the Department of Physical Therapy and Athletic Training in the College of Health, Hicks-Little continues to investigate the consequences of early onset arthritis in the knee joint while examining the effectiveness of different interventions to slow the inevitable deterioration. Now, in collaboration with the Brain Institute at the University of Utah, her research is also focused on another part of the body—the brain and head. Hicks-Little and her collaborators will be tracking brain health and head injuries in collegiate athletes over their careers. “Our group has just received Pac-12 grant funding to examine football and basketball athletes over their collegiate careers to investigate their brain health during sport participation,” said Hicks-Little.
For Hicks-Little, there are definite benefits from working at an academic medical center. “Everything you need to be successful is here and there are so many talented individuals you can collaborate with, learn from, and bounce ideas off. I think that is definitely what drove me to a career in academia,” Hicks-Little states. “Additionally, having the opportunity to interact daily with students to mentor them and develop the next generation of scientists is inspiring and enjoyable.”

GIAVONNI M. LEWIS, M.D.
ASSISTANT PROFESSOR (CLINICAL) OF SURGERY
Research has been a part of Giavonni M. Lewis’ career path from the beginning. During her undergraduate education, she participated in minority research training programs during the school year and research enrichment programs in the summer. After graduating, she participated in post-baccalaureate research at the NIH. Then she realized that her interests lay in the medical field. So she decided to go to medical school, completing a surgery residency and a burn surgery and critical care fellowship.
Now, Lewis is an assistant professor in the Department of Surgery in the School of Medicine, specializing in burn care and translation research. “When I left the NIH, I put research on the side to focus on being a clinician surgeon. And so now I find myself, as I start my career at the University of Utah, really dovetailing into my research. I’m analytical in my approach to clinical care. When I see issues I start to wonder how I can improve care. So translational medicine or translational science is where I live. It’s truly the clinical question that informs my research questions and approach.”
While the burn field is fairly young, there hasn’t been much change in burn care over the past 15-20 years. Lewis’ research focuses on looking for treatment strategies that are practical, logical, and can have a huge clinical impact. For instance, using thermography in a new way to assess burn depth for triage in disaster and rural settings and/or in combination with real-time surgical management in the operating room. Burn surgeons use burn depth to classify burn severity and treatment options but it’s not a precise process. “Unfortunately, we as burn surgeons, are only 60%-70% accurate in determining the depth of burn. Thermography is about 87% accurate. So thermography could be a great tool to provide the burn clinician with a significant amount of accuracy and objectivity and impact surgical management of burn injuries.”
For Lewis, choosing to work at an academic health center was an anticipated option; most regional burn centers are associated with an academic health center due to the amount of support required to deliver multidisciplinary care. But it has provided the working environment that Lewis was looking for and, with support from the Department of Surgery and the Surgical Research Core Laboratories, a place to complete her research.

LORI GAWRON, M.D., M.P.H.
ASSISTANT PROFESSOR (CLINICAL) OF OBSTETRICS AND GYNECOLOGY
Lori Gawron started her career path as registered nurse working in a neonatal intensive care unit. But then she decided that she wanted to have a procedural skill set and to do more research so she applied to medical school. After completing a fellowship in family planning and a master’s degree in public health, she is currently an assistant professor in the Department of Obstetrics and Gynecology.
Like many clinicians, Gawron’s interest in helping medically complex women make reproductive planning decisions was inspired by what she saw in the clinic. “You see adverse pregnancy outcomes happen. Delivering babies who have congenital abnormalities because the woman’s diabetes was poorly controlled. Seeing women get really sick during pregnancy because their disease was poorly controlled going into it. It can affect the woman, it can affect the baby, and it can affect the pregnancy outcomes.”
Gawron’s research focuses on helping providers identify medically complex patients, women with a chronic disease and an increased risk of adverse pregnancy outcomes, so they can assist the patients with reproductive planning. Since reproductive planning is not routinely discussed in all visits, there’s a national push to include it in electronic health records and make it part of preventive health care. “As an ob/gyn, people come into me knowing that they’re probably going to talk about those issues. But they don’t see me as frequently as they might see their gastroenterologist or whoever it is if they have a chronic disease. And so these are missed opportunities.”
Gawron is working with the biomedical informatics group at the University of Utah to develop tools that will work with any electronic health record and help providers identify medically complex patients. Gawron is also collaborating, through research and clinical care, with the VA Salt Lake City Health Care System to provide reproductive planning for service women and develop tools for their system.
Working at an academic medical center has been a perfect fit for Gawron. “I think I’m lucky that I like everything about academia. I love patient care. I love research. I love education. I like the administrative roles that seem to happen in academia, how you can really change departmental culture and also have interactions with all the other subspecialties, not just be in your bubble. And I think that you have a stronger voice for patient advocacy, too.”

YELENA WU, PH.D.
ASSISTANT PROFESSOR OF FAMILY AND PREVENTIVE MEDICINE
Yelena Wu might be a clinical child psychologist and behavioral scientist now but she started out as a molecular cell biology major. In college, she was taking pre-med classes and loved learning about cell science. But then she paused. “I reached this point in sort of my sophomore/junior year where it was time to start making decisions. And I put this sign on my computer that said, ‘What do I enjoy thinking about?’ And I realized that although I love the science and I love medicine, what I really like thinking about is how do people actually cope with health and illness.” This epiphany inspired her to volunteer as a support group facilitator for kids whose parents had recently died, where she discovered her passion for working with people in that way, leading her to major in psychology.
Wu has always been interested in adherence to medical recommendations and finding ways to increase patient adherence to help achieve the best health outcomes possible. As an assistant professor in the Department of Family and Preventive Medicine and an associate member of the Cancer Control and Population Sciences Program at the Huntsman Cancer Institute, Wu’s current primary research is in melanoma prevention. Utah has the highest incidence of melanoma in the country and a large population of people with mutations in CDKN2A/p16, a gene associated with increased melanoma risk. Wu and her collaborators have developed, and are testing, a Skype-based intervention to communicate the idea of melanoma family risk to kids and teach families behavioral and organizational strategies to help increase their adherence to preventive behaviors. “There are so many interesting issues from a behavioral scientist point of view. I realized that so much of what we know is how to help people who already have an illness like asthma and conditions like that. But how do we help kids who need to change their behavior now for something 30 years down the road?”
It’s this balance of clinical care and research that attracted Wu to an academic medical center. “I knew that I always wanted research to be part of my career so I chose institutions that had a really strong emphasis in that area. But I also wanted to remain open to incorporating more clinical service to my work so I looked for institutions that had equally strong opportunities on both the research and clinical sides. I learn so much from working with families clinically that could really inform my research. So if I focus on some of these high-risk populations, for example, I’m going to learn a lot that may extend to other populations, and hopefully in the course of my research, help people in the meantime.”

VANESSA STEVENS, PH.D.
RESEARCH ASSISTANT PROFESSOR, INTERNAL MEDICINE, EPIDEMIOLOGY
It’s always been about infectious disease for Vanessa Stevens. Ever since learning about antibiotic resistant bacteria in her medical microbiology class, she’s been hooked. “SARS (severe acute respiratory syndrome) was emerging when I was in graduate school and I was taking a virology class and thought it was so fascinating,” Stevens related. “So I was very interested in outbreak investigation and that, of course, included hospital outbreaks and antibiotic resistance emergence. And I just started sort of following these things over time.” Stevens experimented with laboratory work during her undergraduate studies but realized that it wasn’t for her and switched her attention to public health. She completed a PhD in epidemiology and a post-doctoral fellowship in pharmacoepidemiology and health outcomes.
Now, as research assistant professor in the Division of Epidemiology in Internal Medicine, Stevens continues to be interested in disease outbreaks. Stevens’ research is focused on promoting the appropriate use of antibiotics for treating infections and reducing the impact of health care-associated infections. “The majority of my research is done at the VA and there are people from all different backgrounds who come together to study infectious diseases. We’ve got cognitive sciences, survey methods, simulation modelers, statisticians, clinicians, and epidemiologists. Every day I learn something new. It’s fantastic to be on the cutting edge of research in a particular field.”
For Stevens, working in academia provides her with the freedom to study what she wants and the flexible schedule that she needs. “Academics is far and away the best place to do things that are new, that are risky, that are cutting edge. Academics is the venue in which you’re constantly striving to keep up with the science,” Stevens shared. “Academics is a great choice for a woman. It’s hard but you know but it’s also flexible which is the thing that you need in order to successfully or at least semi-successfully manage all of the things that you need to do in your life.”

LILLIAM M. PINZON, D.D.S., M.S., M.P.H.
RESEARCH ASSISTANT PROFESSOR OF DENTISTRY
To say that Lilliam Pinzón is a multitasker would be an extreme understatement. She is a research assistant professor in the School of Dentistry and section head for Public Health and Global Health. Since 2005, she’s completed a MS degree, a post-doctoral fellowship, a MPH degree, and advanced training in clinical research. She’s developed seven courses at the School of Dentistry and serves on 10 committees. And somehow she still finds time to work on her research on oral health in underserved populations in Mexico and Columbia. But this career path is where she has always wanted to be. “My main dream was always to be what I am,” Pinzón stated. “Since I was really little, I told my mom that I wanted to be a dentist.”
Pinzón’s research focuses on the use of atraumatic restorative treatments to repair cavities in teeth in vulnerable populations. This technique is done with hand instruments and doesn’t require electricity or water. After removing infected material from the tooth, a glass ionomer treatment is applied that releases fluoride to help harden the tooth. Pinzón is studying the impact of this treatment over time in two vulnerable populations, families in an isolated village in Columbia and HIV patients in Mexico.
For Pinzón, academia has been the only place she has wanted to be. “I worked for a little while in private practice but I love doing research so for me it was more interesting to work in academia. Then I could learn more and create science,” Pinzón related. “It’s a little bit difficult for me. Because I have a lot of responsibilities now, administrative because I’m section head and I have all these courses and committees. But being able to do my research, for me it means a lot because that’s my passion. I love doing research.”

KAREN GIBBINS, M.D.
ASSISTANT PROFESSOR OF OBSTETRICS AND GYNECOLOGY
Karen Gibbins’ interest in research began while working with women during her obstetrics and gynecology (OB/GYN) residency. During that time, she saw several patients with severe early preeclampsia, a condition that raises the mother’s blood pressure and can decrease blood flow to the placenta. “When preeclampsia happens at an early enough gestation before the baby can survive, you have to induce and you lose the pregnancy,” Gibbins explained. “Those are things that you take home with you. And they stay with you. If there’s something you can do to help, you want to do it.”
Now, as an assistant professor in the Division of Maternal-Fetal Medicine in the Department of Obstetrics and Gynecology, Gibbins has taken inspiration from her experiences in clinical care and applied it to studying the placenta, one of the least studied human organs, and what contributes to abnormal development. If the placenta isn’t working properly, it can result in problems ranging from stillbirth to preeclampsia to fetal growth problems. Currently, there is no way to predict when the placenta will malfunction and no tools to fix it when it does.
“Preeclampsia and fetal growth problems are treatable but we don’t have any treatments to make them better besides monitoring closely and then delivering when we think things are about to become even worse. So it results in preterm birth most of the time. If we could come up with some sort of treatment that could either prevent stillbirths or allow women to continue their pregnancies further, that would be huge.”
During her career, Gibbins was always impressed by clinician scientists so it’s not surprising that she chose to work at an academic medical center. “I’ve always loved the clinical side of OB/GYN and high risk pregnancy but I’ve always wanted to do something that affects more beyond the individual patient interaction. And that’s where research comes in. I like having the mix. I like that I get to go to clinic and do ultrasounds and work on labor and delivery but then also go to research meetings and think of new ideas and talk to my colleagues. And the idea that I could make a contribution that would ultimately go on to better care for large amounts of women and children, that’s what’s exciting about it.”

JUNE ROUND, PH.D.
ASSISTANT PROFESSOR OF PATHOLOGY
If it hadn’t been for the inspiration she received from her college courses and professors, June Round might have been an FBI agent by now. When Round started college, she was a criminal justice major with no interest in science. Then she took a general biology course and the light bulb flickered on. “It was that experience, taking those classes that made me realize that I liked biology,” Round stated. “I liked science. And it just clicked for me. Whereas the criminal justice classes, history classes, that stuff…I would fall asleep in those classes.” After changing her major to biology, Round completed her science education with a master’s degree in molecular biology and a PhD in microbiology and immunology.
It was during her PhD work that Round became interested in her current research, studying the links between the immune system and the commensal, or non-harmful, bacteria that saturate our bodies. Specifically, Round studies how these bacteria interact with our immune system and help promote healthy immune system responses. “I always thought of us as very sterile creatures but that’s not true. The minute we come into the world, we are born with these bacteria. We’re swimming in a sea of microbes that our immune system totally ignores or actually actively tolerates. I’m fascinated by how we could have studied the immune system for decades and ignored this very basic, and probably very important, interaction between microbes and the immune system.”
As an assistant professor in the Division of Microbiology and Immunology in the Department of Pathology, Round opted to work at an academic health center for the creativity and the freedom that is here. “I started my lab studying inflammatory bowel disease, but we have since branched out to the central nervous system because there’s very collaborative people here at Utah. There’s not that restriction [in academia] so you have the freedom to get into new, exciting areas.”

HEIDI HANSON, PH.D., M.S.
RESEARCH ASSISTANT PROFESSOR OF PUBLIC HEALTH; UTAH POPULATION DATABASE; HUNTSMAN CANCER INSTITUTE
You can call her a data geek but Heidi Hanson won’t mind a bit. As a research assistant professor in the Division of Public Health and population specialist with the Utah Population Database (UPDB), Hanson thrives on data. “I love data,” Hanson explained. “I’m a huge data geek. Nothing makes me more happy then when we get big datasets.” After getting her bachelor’s degree, Hanson worked for the UPDB but left for a career opportunity in the private sector. When that didn’t fit with her career path, she returned to work with the UPDB and went to graduate school to get her PhD.
Hanson’s research uses large datasets in the UPDB and statistics to find patterns of disease. “I’m trying to figure out the exposures throughout the life course, environmental and genetic, that contribute to the way that we age and get disease,” Hanson stated. One topic that Hanson is studying is family patterns of increased cancer risk and identifying the factors from birth to death that contribute to that risk. “I’m really interested in the life course perspective, which investigates how exposures as early as in utero affect the way we age later in life. A large proportion of my research focuses on cancer risk because many cancers have a long latency period. It is essential to understand how exposures early in life lead to adverse health outcomes later in life.”
For Hanson, working in an academic health center has allowed her the freedom to really explore different ways of looking at things. Hanson elaborated, “I absolutely love what I do. However, part of me loving what I do is the fact that I had the ability to grow in directions that I wanted to or needed to in order to progress my research.” Working in an academic health center has also provided Hanson with the opportunity to work with people from multiple fields, something that she believes is important in order to do good science. “Sometimes you become so focused on your ideas that you forget to really question them. That’s why collaborations from multiple disciplines are so important. Including multiple points of view, from physicians, sociologists, computer scientists, and other academic disciplines, is essential to furthering knowledge. Good science can’t be done until we start to really approach it from a multidisciplinary standpoint.”

TRUDY OLIVER, PH.D.
ASSISTANT PROFESSOR OF ONCOLOGICAL SCIENCES, HUNTSMAN CANCER INSTITUTE
Trudy Oliver knew that she wanted to go to college but, as a first generation college student, she wasn’t sure what that looked like. “I grew up in Oklahoma on a farm and my parents didn’t graduate from college so I didn’t know a whole lot about academic anything.” But, once she got there, Oliver had mentors that guided her into summer research programs and a PhD program in cancer biology.
Now, as an assistant professor in the Department of Oncological Sciences and an investigator at Huntsman Cancer Institute, Oliver has developed squamous and small cell lung cancer mouse models in order to test drug responses and drug resistance and identify new treatment therapies. “In lung cancer, like in other types of cancer, there are multiple types. And even when you have a certain type of lung cancer, it doesn’t mean that yours would behave the same as mine even if it were the same type. If you put any kind of stress on it, the ones that have resistance to whatever your threat is, those survive and grow up and take over…Cancer is the ultimate chameleon.”
For Oliver, working at an academic medical center gives her the opportunity to be her own boss. “There is a hierarchy but by and large, I decide everything. From when to get up, to when to stop, to what we’re going to work on, to who I hire, to when we change directions. All of it.” But it also allows her to be able to follow her passion for doing science wherever it takes her. “There’s nothing more exciting then when you figure something out based on reason, that you’ve really worked hard at, and you’re the first person in the world to have discovered that. That’s just an amazing feeling. And it’s much more of a pure endeavor in that we’re seeking knowledge not always for a product or to make money. But what we do has the potential to help people.”

DEANNA KEPKA, PH.D., M.P.H.
ASSISTANT PROFESSOR OF NURSING, HUNTSMAN CANCER INSTITUTE – DIRECTOR OF THE INTERMOUNTAIN WEST HPV VACCINATION COALITION
Deanna Kepka has always been interested in disparities, those differences in education, resources and health care that can exist between two different populations. But it wasn’t until she was a Peace Corps volunteer studying nonprofit management that she realized she was interested in research and public health. “I worked on a project to improve healthy lifestyle choices to prevent HIV infection among at-risk youth. While I was there, I decided to do an evaluation of the program I was working on. I wrote an abstract for the International AIDS Conference and won a scholarship to go and present that research. So that kind of exposed me to the world of research and got me more into public health.”
Now, as an assistant professor in the College of Nursing and an investigator at the Huntsman Cancer Institute in Cancer Control and Population Sciences, Kepka seeks to reduce cancer health disparities by trying to increase cancer screening and cancer prevention behaviors among vulnerable populations. She also serves as team leader for the Health Disparities and Cancer Prevention (HEDCAP) group within Cancer Control and Population Sciences.
As director of the Intermountain West HPV Vaccination Coalition, Kepka’s research focuses on improving the rates of human papillomavirus (HPV) vaccination. “The Intermountain West is a region with some of the lowest rates of HPV vaccination in the United States,” Kepka explained. “HPV is the most common sexually transmitted infection and we have this cancer prevention vaccine that is severely underutilized. So it just seemed like a really important health issue.” She is also collaborating with Lilliam Pinzon from the School of Dentistry to assess dental student knowledge about HPV-related head and neck cancers and their attitudes towards recommending the vaccine to their patients when they become practicing dentists.
Working at an academic medical center allows Kepka to act as a bridge from the latest science to the vulnerable communities she’s trying to help. “I really enjoy the stimulation and being at the heart of where science happens,” Kepka shared. “But then disseminating the best strategies we know to prevent cancer to communities. I like having that role. What’s the point in developing all these different innovative strategies to prevent cancer if they’re actually not being used? I like to make that happen.”

CINDY BROWN MATSEN, M.D.
ASSISTANT PROFESSOR OF SURGERY
Growing up with a father who was a family practitioner, Cindy Matsen knew from a very young age that she wanted to be a doctor. But it wasn’t until her third year of residency that she decided to be a breast surgeon. “It was because I had mentor here who was a breast surgeon and I realized that I really liked what she did,” Matsen explains. “I like doing low risk, high impact surgery, which is what breast cancer surgery is. I like having longer-term relationships with my patients. And I really like complex decision-making, which is where the research part really comes in.”
Matsen, an assistant professor in the Department of Surgery in the School of Medicine, splits her time between working with patients and conducting research on how doctors and patients communicate and how to improve that communication. “I’m really interested in how doctors and patients talk to each other and how they make decisions together.”
Matsen uses qualitative and quantitative methods to study the techniques doctors use when communicating with patients and to see how changes to those techniques can impact decision-making. She believes that doctors, by making small behavioral changes in how they communicate with patients, can have major impacts on health. “I think we often think we have an inherent understanding of who somebody is when they walk in the door but we have no idea. We have medical information but we have very little information on who they are as a person and what’s actually important to them. And if we did a better job of recognizing those things, I think that our outcomes would be a lot better.”
By working at an academic health center, Matsen was able to combine her interests in clinical care and research into one career. “There’s always new things happening, especially in breast cancer, but I feel like research gives you another outlet. It kind of gives you a creative outlet to really think about, ‘Okay. If I think this is a problem, how would I fix that? How can I make this better?’ And I like that idea. That’s the thing I like in academic medicine is that it’s about improving things. You have a much broader impact when you do research. You can actually change things for your whole field.”